




Wellcare Insider: Important Updates and Reminders
CustomPoint Ordering
When requesting sales materials through the CustomPoint portal, a complete address is necessary to ensure accurate and timely delivery of your materials.
- Review all delivery address information prior to submitting your order.
- Suite or Apartment designations and numbers must be entered to ensure delivery accuracy.
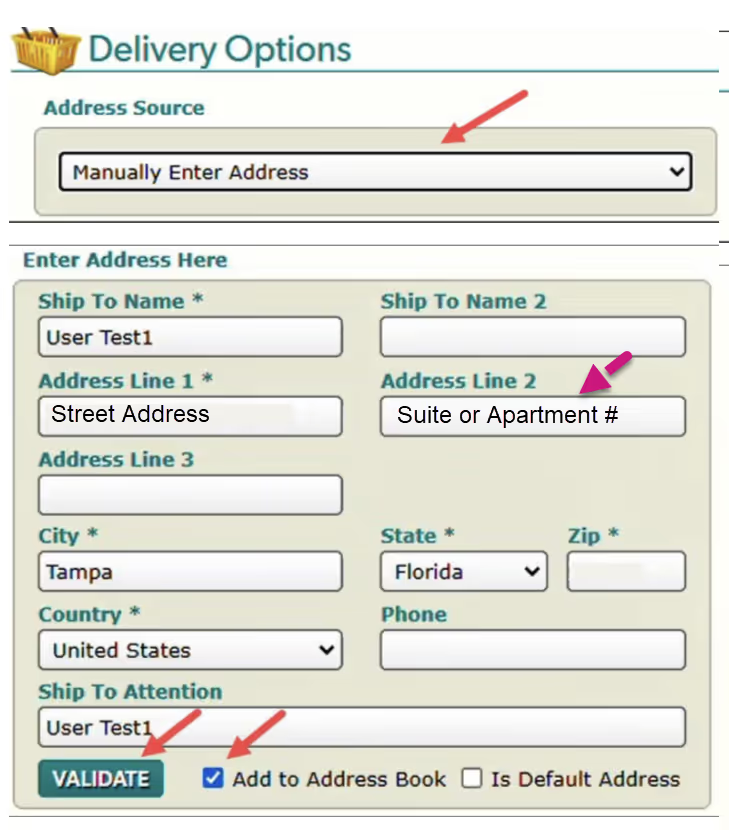
- Select Manually Enter Address to correct any missing information.
- Utilize the Address Line 2 field as shown in the example to the right to designate whether the address contains a Suite or Apartment and enter the number information.
- Validate and select Add to Address Book to complete your address update.
ICYMI - Emergency/Disaster SEPs Extended to Six Months
As previously communicated, a CMS ruling has extended the duration for any Special Enrollment Period (SEP) arising from an emergency or disaster declaration occurring on or after January 1, 2023.
What this means: Previously the guidance allowed the SEP to last the entire incident period plus 2 months after the end date of the incident period. After this recent change, the SEP is now available from the start of the incident period until 6 months after the end of the incident period.
What you should do now: Visit Special Enrollment Period (SEP) - FEMA / State Declarations to see if there is an active disaster SEP declared in your state. Note that previously expired SEP notifications have been updated as a result of this ruling.
Agent of Record Promise
Wellcare strives to be a leader in the industry and your trusted partner in business. You can have confidence that when you speak, we listen. Our Agent of Record Promise (AOR) commitment recognizes that you work hard, deserve the commissions you earn, and we promise to protect your commissions for members you have enrolled.
You can rest assured, when an existing client makes a plan change by calling Wellcare directly, your AOR status will remain unchanged. This means you will remain the AOR and continue to receive renewal commissions on plan changes. This even applies to plan changes from PDP to MAPD, where applicable. The Agent of Record Promise benefits your book of business year-round.
Take a moment ahead of the upcoming sales season and review the AOR to learn more about our commitment and the benefits for your business.
Questions? Call us at 855-888-8326.
Don't have a MedicareValue page yet?
Get Your FREE Site >Posts you may be interested in...
 Read More
Read MoreMeet your California Broker Channel Manager: Sandy Wang
Meet your new Broker Channel Manager in California!
 Read More
Read MoreNew business technology is on the way for brokers!
These changes include a new contracting system for all brokers/agents, and a new commissions experience for MA/PDP users.
 Read More
Read MoreHighmark Important Updates: Medigap, SSBCI, and Delaware D-SNP Information
Medigap, SSBCI, and Delaware D-SNP Information
 Read More
Read MoreExtend Your Molina Selling Season to December 31!
AEP is coming to a close, but the Integrated Care SEP* can still be used
 Read More
Read MoreUnitedHealthcare: JarvisWRAP for December 1
AEP support, UCard shipments and SSBCI verification
 Read More
Read MoreCigna Broker Insights: November 2025 - Edition 11.2
Broker Insights: The newsletter for all Medicare brokers - 11.2
-01.png)
Who we are & what we do.
Choosing an FMO to work with is not just about having access to top insurance products and commissions, it’s about finding a one-on-one agent service that is prepared to meet your needs.
Get to know us, and see how we can help you take your business to the next level.

.svg)








